Ongoing research shows cannabis plays a role in gastric motility. Gastric motility is the action by which food travels through the digestive tract. The process is controlled by a series of muscles that line the digestive tract, causing muscular contractions known as peristalsis. When peristalsis is functioning normally, food moves from the mouth to the stomach, small intestine, large intestine and exits through the anus. Stomach acids and bile aid this process.
Peristalsis is a wave-like kind of muscle contraction that moves solids and liquids through the digestive tract. It’s not a voluntary muscle movement, meaning it’s not something a person can consciously control. The muscles operate when stimulated by food consumption. When peristalsis is not functioning – a condition called gastric dysmotility – it can cause a range of symptoms that vary in severity. The most common symptoms include diarrhea and constipation.
To stay current on everything important happening in the industry, as well as gain access to deals on cannabis flowers, vapes, edibles, and much more (various cannabinoids to choose from), make sure to subscribe to The Cannadelics Weekly Newsletter. Enjoy responsibly!
Causes of Motility Disorders
Peristalsis works in a coordinated and orderly manner to transport food from the mouth to the stomach. In the stomach, food is converted to a substance called chyme, that is then moved through the intestines and finally, to the anus where it is excreted. A disorder or dysmotility results in either too slow and/or too fast movement of food through the gastrointestinal (GI) tract.
Any change in the speed of movement can cause symptoms. Motility disorders can occur as a result of dysfunction of the nerves and/or muscles in any region of the GI tract. If the muscles are not working correctly, it’s known as myopathy. When the nerves are affected, the conditions are related to neuropathy. The exact cause is often unknown. Dysmotility may present on its own or be linked to another underlying condition. In some cases, the condition is hereditary.
Types of Motility Disorders
Types of motility disorders vary depending on which area of the GI tract is affected by the condition. The following are the most common conditions associated with motility disorders.
Gastroparesis
Another term for gastroparesis is “delayed gastric emptying,” a condition where the stomach is slow to empty chyme. Once food has been digested, a healthy stomach will move chyme into the small intestine. When the nerves that control the stomach are damaged, causing food to move too slowly, it will cause symptoms including nausea, burping, bloating, heartburn, indigestion, regurgitation and/or vomiting. Gastroparesis is linked to diabetes, which accounts for one-third of cases. The opposite also exists, where food empties too quickly, a condition called dumping syndrome or rapid gastric emptying.
Irritable Bowel Syndrome
Irritable bowel syndrome (IBS) affects the functionality of the digestive system, altering motility. In some cases, motility is too fast, leading to chronic diarrhea (IBS-D), or in others, too slow, causing chronic constipation (IBS-C.) It’s also possible to have a mix of both diarrhea and constipation, known as IBS-M. Other symptoms include pain, bloating and fatigue.
Esophageal Spasms
Esophageal Spasms are irregular contractions of the muscles in your esophagus, the tube that leads from the mouth to the stomach. The cause is unknown, but the symptoms include chest pain, which can sometimes be mistaken for a heart attack.
Hirschsprung’s Disease
Hirschpring’s disease is a congenital disorder, leading to poor motility that causes a blockage in the large intestine. It’s more common in males than females and is sometimes linked to inherited conditions such as Down syndrome.
Gastroesophageal Reflux Disease (GERD)
GERD is a condition where the contents of the stomach move back up the esophagus causing heartburn and reflux. It can also lead to difficulty in swallowing, chronic cough, bad breath, and if left untreated, can lead to further complications.
Small Intestine Bacterial Overgrowth (SIBO)
SIBO, as the name suggests, is the presence of too many bacteria in the small intestine, leading to motility issues, and other problems including pain, bloating, gas, fecal incontinence and nausea.
Cannabinoids in the GI Tract
In the 1980s, the discovery of the endocannabinoid system (ECS) led to a new understanding of human physiology. More recently, it’s led to a new understanding of gut health. The ECS is made up of CB receptors that are located throughout the body. CB1 receptors are found in the GI tract, predominantly in the myenteric (nervous system in the small intestine) and submucosal neurons (regulators of water and electrolyte secretion and blood flow in the gut), and in non-neuronal cells such epithelial cells (type of cell tissue found on surface of organs and blood vessels.)
CB2 receptors are found in the immune system, and are present in the gut as part of an inflammatory response. Endocannabinoids or cannabinoid ligands (messengers) activate CB receptors. Two of the main endocannabinoids identified in mammalian tissue include anandamide and 2-arachydonylglycerol (2-AG.) Endocannabinoids are produced on demand, activating biological responses. Following activation, they are de-activated through an enzymatic process that provokes further biological responses. Each of these responses has implications for gut health.
Current understanding of cannabinoids and endocannabinoids relies heavily on findings from animal studies. The following is a summary of the major functions of cannabinoids in the GI tract:
- Cannabinoids are anti-nociceptive (pain-blockers.)
- Cannabinoids inhibit GI motility through CB1 receptors in physiological conditions, and through CB1/CB2 receptors during inflammatory response.
- Phytocannabinoids repair intestinal permeability during inflammation or after exposure to toxins.
- Activation of CB1 receptors reduces acid secretion in the stomach.
- Cannabinoids induce hyperphagia (increased appetite) resulting in weight gain.
- Cannabinoids reduce nausea and vomiting, and are anti-inflammatory.
- Cannabinoids have anti-cancerous and anti-bacterial properties.
Therapeutic Uses of Cannabinoids on GI Motility
Further research needs to be undertaken to define and refine the therapeutic uses of cannabis and cannabinoids in treating GI disorders. However, what’s known as a result of animal studies and human studies (with less than 20-30 participants) is that cannabinoids affect motility by direct action on the GI tract and indirect action via the nervous system.
In fact, it’s been known for decades that cannabinoids reduce intestinal motility. However, more recently that it was discovered this action is due to the activation of CB1 receptors, an effect which is counteracted by the selective CB1 antagonists, rimonabant. An agonist is a chemical that activates a biological response, whereas an antagonist blocks a biological response.
For example, due to their effects on motility and secretion, CB1 agonists might be useful to treat IBS-D, whereas CB1 antagonists could be useful to treat IBS-C. Also, activation of CB2 receptors, which are present during inflammation, may be useful to treat IBS-D. To treat GI sensitivities, a possible solution could be a type of enzyme-blocker that raises anandamide levels.
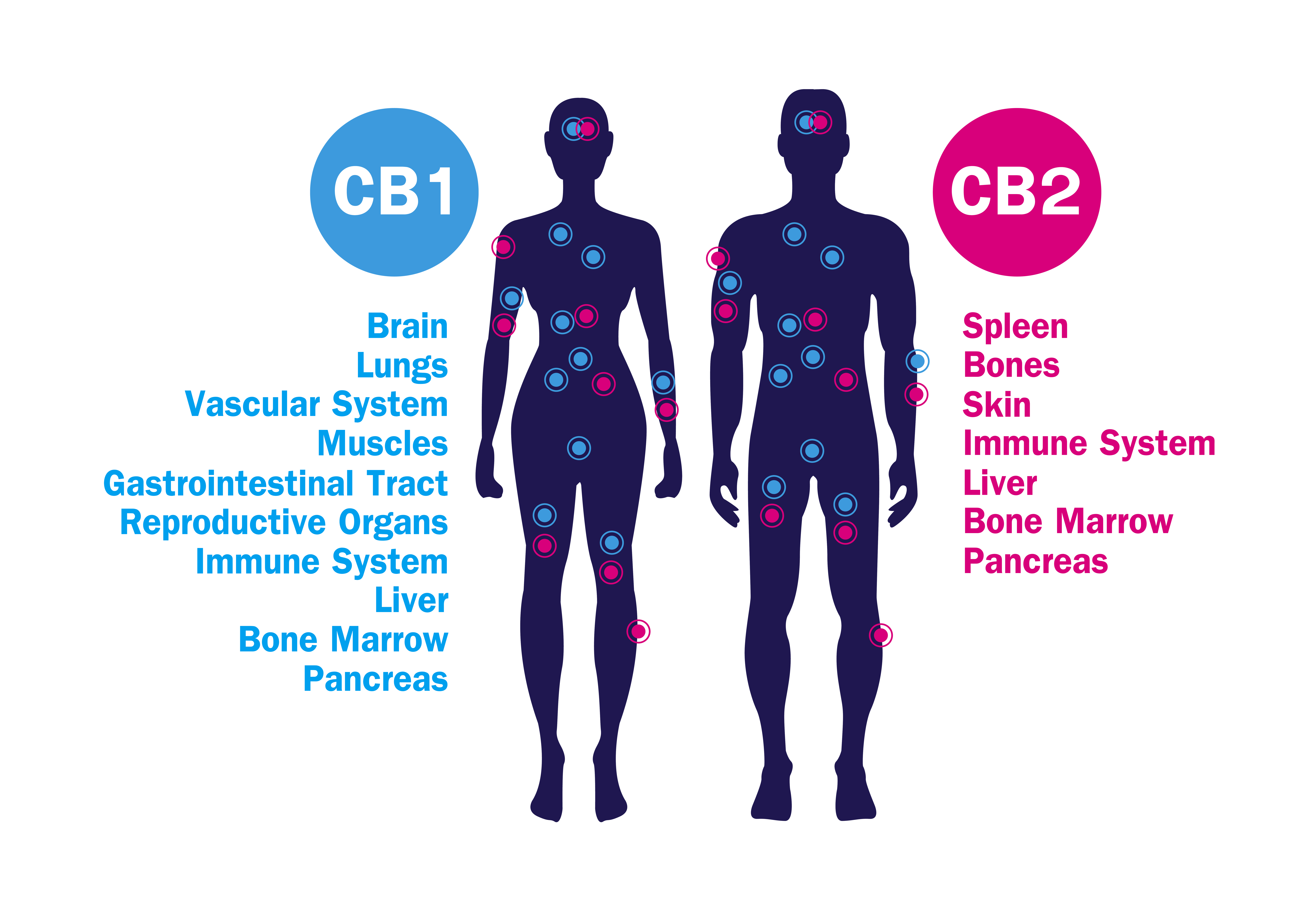
As both CB1 and CB2 receptors are present on the gut-brain axis and are involved in triggering of the lower esophageal sphincter relaxations, it suggests a possible treatment for esophageal spasms. In a study on guinea pigs, activation of CB2 receptors reduced microvascular leakage. Therefore, an increased CB tone could inhibit gastro-esophageal reflux along with adjunct therapy.
On top, it’s believed that changes in levels of endogenous cannabinoids during inflammation may contribute to motility issues. Depending on the site of inflammation, both CB1 and CB2 receptors may reduce the hyper-motility associated with gut inflammation. In some animal studies, hyper-motility was completely normalized by a CB2 receptor agonist.
Final Thoughts
The human body is complex, and the discovery of the ECS, which acts as a modulator between the digestive, immune and nervous systems adds to that complexity. However, it also opens the door to new fields of research that can offer solutions to a range of gastric conditions. For now, more work needs to be done to offer patients reliable treatments, but due to the high number of people with motility disorders, this issue is of huge interest to researchers. It’s not unreasonable to expect major breakthroughs in this field in the near future.
Hello readers! We appreciate you joining us at Cannadelics.com, a top choice news platform for independent coverage of the growing cannabis and psychedelics landscapes of today. Come by the site whenever possible for updates on current and world-changing events, and head over to the Cannadelics Weekly Newsletter, so you’re always up on what’s going down.










Which cannabinoids can help motility? CBD? Delta (#) THC? CBN? There are a lot of them, which one helps?
As explained, further research is needed to offer specific advice. Also, bear in mind, each person will experience a different effect. And yes, there are more than 400 biologically active compounds in the cannabis plant, lots of research needed!!!